
Choose your most prominent symptom:


Fungus and sinusitis
I've been surprised by how many patients ask me about the link between fungus (mold) and their sinus problems. Most of the questions come from a Mayo Clinic study from several years ago and the news coverage that followed. The study basically concluded that most long-lasting sinus inflammation (chronic sinusitis) was related to fungus.
The truth is there is a lot we still don't know about long-lasting sinus inflammation. It almost certainly has several different causes, even though it tends to look the same when patients walk in. Many cases probably have more than one cause working together. It has now been clearly shown that fungus plays a much bigger role than we used to think. The most common type of fungal sinusitis is called "allergic fungal sinusitis." It's not really an allergy, but the name has stuck. Let's look at a few things about sinusitis and the role fungus plays in it.
What is fungal sinusitis?
Fungal sinusitis comes in several well-described forms, plus some forms we are just starting to learn about. They fall into 4 groups:
1) The most obvious is invasive fungal infection — for example, invasive mucor — where a person with a weakened immune system gets a life-threatening infection that grows into the tissues. I have never seen a case in my practice.
2) Next is what's called a fungus ball. It's usually in one sinus, most often the cheek sinus (maxillary sinus), and is a clump of fungal threads. It doesn't grow into the tissues and doesn't cause much inflammation. Symptoms vary and are usually mild. Treatment is to remove the fungus ball. This is fairly common and usually only affects one sinus.
3) About 7% to 10% of long-lasting sinusitis patients who come to surgery have a fairly well-defined condition called allergic fungal sinusitis. It is an inflammatory reaction to non-invading fungus — a fungus that is in everyone's nose, but that only some people react to.
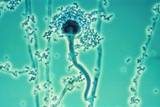
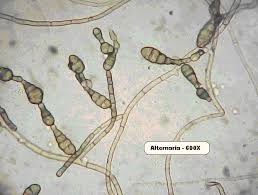
It isn't really just an allergy. More parts of the immune system are involved than with the usual breathed-in allergies. The problem starts when certain people's immune systems "overreact" to mold spores like Alternaria and others. These are types of common mold. Some people react in a way that leads to swelling, polyps (growths in the nose lining), and secondary infection. The reaction happens in the mucus, not in the nose tissues themselves. The most typical finding is a large amount of so-called "allergic fungal mucin" — a thick, sticky goo in the affected sinus that contains fungal threads and immune cell debris. Fungus can often be grown from a sample. People with this condition almost always have polyps, and it is often only on one side.
The CT scan often has a typical look, with mixed-density patches inside the sinus — sort of marbled. Treatment includes surgery to clean out the allergic fungal mucin, opening wider drainage paths, steroid pills around the time of surgery, and careful follow-up afterward with frequent cleanings, steroid pills for any sign of return, and long-term use of anti-fungal nose rinses or sprays.
The outlook is not as good as for most other causes of long-lasting sinusitis. More patients have it come back, and more eventually need a second surgery to clean out built-up fungal material and recurring polyps. Steroid pills work remarkably well, and the key to treatment is good surgery plus careful balancing of how much steroid to use, since steroids have side effects but help so much.
Anti-fungal nose rinses and sprays have recently been shown to help, and I now use them routinely in patients with clear-cut allergic fungal sinusitis.
4) A lot of long-lasting sinusitis that ends up needing surgery, but isn't clearly allergic fungal sinusitis, has recently been shown to be a milder version of the same process. This is helpful because it explains why some people don't do as well after surgery as we hoped, and it tells us what to try if those patients have problems afterward.
Things we still don't fully understand about fungal sinusitis:
1) Many — but not all — long-lasting sinusitis cases can be cleared up completely with the right long course of antibiotics and supporting medicines. If that's true, how can fungus be the root cause?
One explanation is that the fungus damages the lining of the nose first, and then bacteria move in and cause the infection. Another explanation tries to relabel this kind of problem as "sub-acute sinusitis" and separate it from true "chronic sinusitis," which some researchers think is entirely fungal in origin.
2) In many clear cases of allergic fungal sinusitis, the problem is only on one side. If the body is reacting to a fungus that is everywhere, why would it only be on one side? The shape of the nose seems to play a role. This may be why we can clear up long-lasting sinusitis with surgery — if mucus can flow more freely, the fungus doesn't have time to grow, and the body sees less of it.
3) Is this reaction to Alternaria and similar molds something you are born with?
4) Does something in the environment trigger it?
5) Once someone has this immune response to Alternaria, is it permanent?
6) Does the reaction come and go over time?
Summary:
Long-lasting sinusitis has several causes. A major Mayo study and recent research show that an immune reaction to airborne mold is much more common than we used to think. The practical takeaway is that anti-fungal nose rinses or sprays can help even in people who don't have a clear-cut case of allergic fungal sinusitis.

Is your problem from mold?
Is fungal sinusitis allergy?
What is mold spore allergy?
Let us help you figure it out.
